What is High-dose-rate (HDR) Brachytherapy for Gynecologic Cancer?
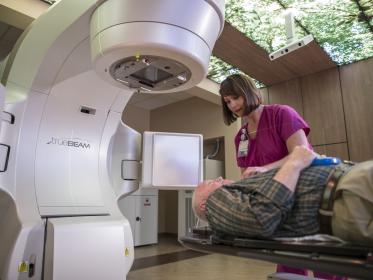
High-dose-rate (HDR) brachytherapy, also called internal or intracavitary radiotherapy, involves placing radioactive sources in or next to the cancer. This is usually done at the same time or after external beam radiation therapy to achieve the best results. Brachytherapy is important in the treatment of vaginal, cervical, and uterine cancers.
High-dose-rate brachytherapy does not require you to be admitted to the hospital. The entire procedure typically takes a few hours. Your office will contact you regarding the brachytherapy treatment dates and times to arrive at the hospital. You will be need someone drive you and you cannot eat after midnight the evening before each treatment.
What Happens on the Day of Your Procedure
You will go to the Registration Office at UT Medical Center, then be taken to the appropriate pre-surgical area. The treatment devices will be placed by the gynecologic oncologist and radiation oncologist in the operating room while you are under anesthesia. A catheter will be placed in your bladder at this time. Once this is complete, there will be a brief stay in the post-surgical recovery area while you recover from the anesthetic.
Next, you will be transported to Radiation Oncology where a CT scan will be done to use for planning that day’s treatment. The planning can take around an hour. You will remain on bedrest until the treatment is completed and the devices are removed. Your family can stay with you during this time, and you may have liquids.
When the treatment plan is final you will be taken to a treatment vault; a long tube (catheter) will be connected to the external part of the vaginal applicator. This will then be connected to the radiation source.
Once devices are connected, the staff will exit the treatment vault while the radiation dose is delivered; this usually takes 10 to 15 minutes. You will be watched by way of in-room cameras, and we can talk to you and hear you. You will not feel any sensation while receiving the radiation.
When the procedure is complete, the physician will remove the devices and catheter and you can go home.Plan on resting the remainder of the day. Because of the anesthetics you were given, do not drive for 24 hours.
Potential Side Effects
The side effects you may experience will depend on the area being treated.
- Some patients experience minor or no side effects, and can continue their normal routines.
- Some patients may notice nausea, fatigue, skin irritation, vaginal irritation and discharge, frequent urination, burning with urination, and diarrhea. These should resolve gradually after treatment ends.
- Some time after your treatment, you may see minor changes to your bowel, bladder, or vagina. Radiation may cause the vagina to be drier and less flexible. Ask your doctor or nurse how to manage these changes. More severe side effects are not common. If you have concerns, please call your doctor to discuss.
- You may have additional side effects if you are receiving chemotherapy at the same time as radiation therapy.
If you develop side effects, tell your doctor or nurse. They can give you medicine to help.
Guide for Coping With Pelvic Radiation Side Effects
- Use prescribed ointment for soreness in small areas.
- Do NOT use diaper rash products or Vaseline products.
- Take warm sitz baths to help clean the area and sooth irritation. You can take up to four sitz baths a day as needed. You can also use a squirt bottle with warm water as a substitute.
- After bathing, pat dry the irritated areas, do not rub.
- Use over-the-counter stool softeners.
- Drink plenty of fluids.
- If you’re feeling a burning sensation with urination, check with your doctor to make sure it isn’t a urinary tract infection. Then ask about a prescription medication for urinary anesthetics (i.e. Pyridium)
If You Need Us
For any questions or concerns, please call our office at 865-305-9040, and ask to speak to the HDR Nurse.