Overview
When you’ve been diagnosed with cancer, it’s important to review your treatment options with your health care team. One possible option for solid tumors is radiation therapy. You should always discuss all options for treating your cancer with your health care team. They can help you decide the best treatment for you.
This patient guide will provide a general overview of the various types of radiation oncology. This includes both radiation therapy (also called radiotherapy) and radiosurgery treatments. Be sure to talk about any questions with your health care team.
Radiation oncology teams use advanced software and very specialized equipment to give patients different types of treatments. Which treatment you get will depend on what’s best for your case. Your radiation oncologist, or cancer doctor who specializes in radiation therapy, will talk with you about your radiation treatment options. He or she will also help you decide which the best one for your particular cancer.
How Does Radiation Therapy Fight Cancer?
Radiation therapy uses focused X-rays, which are a type of energy, to kill cancer cells. Because they are focused, this reduces the risk to your healthy tissue. Radiation damages the DNA in cancer cells. This breaks up their ability to reproduce, which makes them die, shrinking the tumor. Most normal cells can repair themselves and recover from the radiation. If normal cells near the tumor area receive radiation, it can cause some side effects.
Side effects vary from patient to patient. Many side effects can build up over time. This means they can get worse as the radiation accumulates in the tumor. They can be minor or severe, depending on three main things:
- How big the tumor is
- Where it’s located
- How healthy you are
You’re most likely to have two side effects: irritation or damage to the skin near the treatment site, and fatigue. But you may also have more serious side effects. These can include:
- Diarrhea
- Nausea
- Swelling at the treatment site
- Lymphedema (swelling in the arms and legs)
- Secondary cancer
Your treatment team will help you manage any side effects you may experience.
Radiation Treatment Techniques
There are two types of radiation therapy: radiation therapy — also called radiotherapy — and radiosurgery. Neither of these require an incision, or cut. Instead, they focus a beam of radiation right on the tumor while lessening exposure to healthy tissue around it.
There are two main differences between the treatments: how many treatments you get and how strong the radiation is. If you get radiotherapy, you’ll usually have treatment sessions five days a week, for four to six weeks. Each treatment session lasts between two and 15 minutes.
If you get radiosurgery, you’ll have it in five or fewer sessions over one or two weeks. Most treatments will last from a few minutes to 30 minutes. Also, the strength of each dose is much higher in radiosurgery. This makes it a better treatment for deep tumors, small tumors, and cancers that have spread, or metastasized, to other parts of the body.
Each of these two types of treatment can given in different ways. It all depends on what’s most appropriate for you. Here are the most common ways that doctors use radiation.
Types of Radiation Therapy Treatments
Your Clinical Team
A team of specialists will give you radiotherapy. The team may include:
- Radiation oncologist — A cancer doctor who specializes in radiation therapy
- Medical physicist — A scientist who knows the latest information about radiation
- Dosimetrist — The person who decides how much radiation you get and for how long)
- Radiation therapist — The person who gives you your radiation therapy
- Radiation nurse — The person who takes care of you during your treatment
If you’re getting radiosurgery, your team will include:
- Radiation oncologist — A cancer doctor who specializes in radiation therapy
- Neurosurgeon — A doctor who specializes in the central nervous system, or brain and spine
- Specialty surgeons — Doctors who focus on different parts of the body, like a thoracic pulmonologist, who treats lung disease
Whether you’re getting radiosurgery or radiotherapy, you may also have these people on your team:
- Physician assistant — A health care professional who works with doctors to give patients medical care
- Radiologist — Doctors that specialize in radiation therapy
- Dietitian — An nutrition expert
- Physical therapist — A medical expert who helps injured or ill people improve their movement and manage their pain
- Social worker — An expert who supports patients, families and caregivers who are dealing with cancer
- Other people who specialize in the area of the body being treated (like a urologist, or prostate cancer doctor)
Treatment Process
Each type of therapy, radiotherapy or radiosurgery, includes the same basic steps. They are:
- Tumor visualization
- Treatment planning
- Treatment delivery
- Follow up
Your clinical team will decide on the best treatment for you. In addition, they will answer any questions you may have before, during or after treatment.
Tumor Visualization
To design your treatment plan, your treatment team will take images to show the exact location of the tumor. This includes its size and position in relationship to the tissues and organs around it. The team typically does this with a CT scan. Depending on the tumor’s location and other factors, they may also take other scans, like an MRI, PET scan or ultrasound. With the help of these scans or images, your clinical team can see details of the tumor from different angles.
Depending on your treatment, you may have a custom body-mold (or mask if your head is being treated). You may also get tiny skin marks to help make sure you’re in exactly the same position for each session.
Planning
When the scans are completed, your clinical team will use advanced treatment planning software. This will create a 3D, or three-dimensional “picture” of the area where you will get treatment. They’ll determine how much radiation to deliver, the best angle to give it from, and how many sessions you’ll need. They’ll also take into account many other factors, like:
- The type of cancer you have
- Its location and size
- Your medical history
- Your lab test results
They will use this information to create a plan just for you.
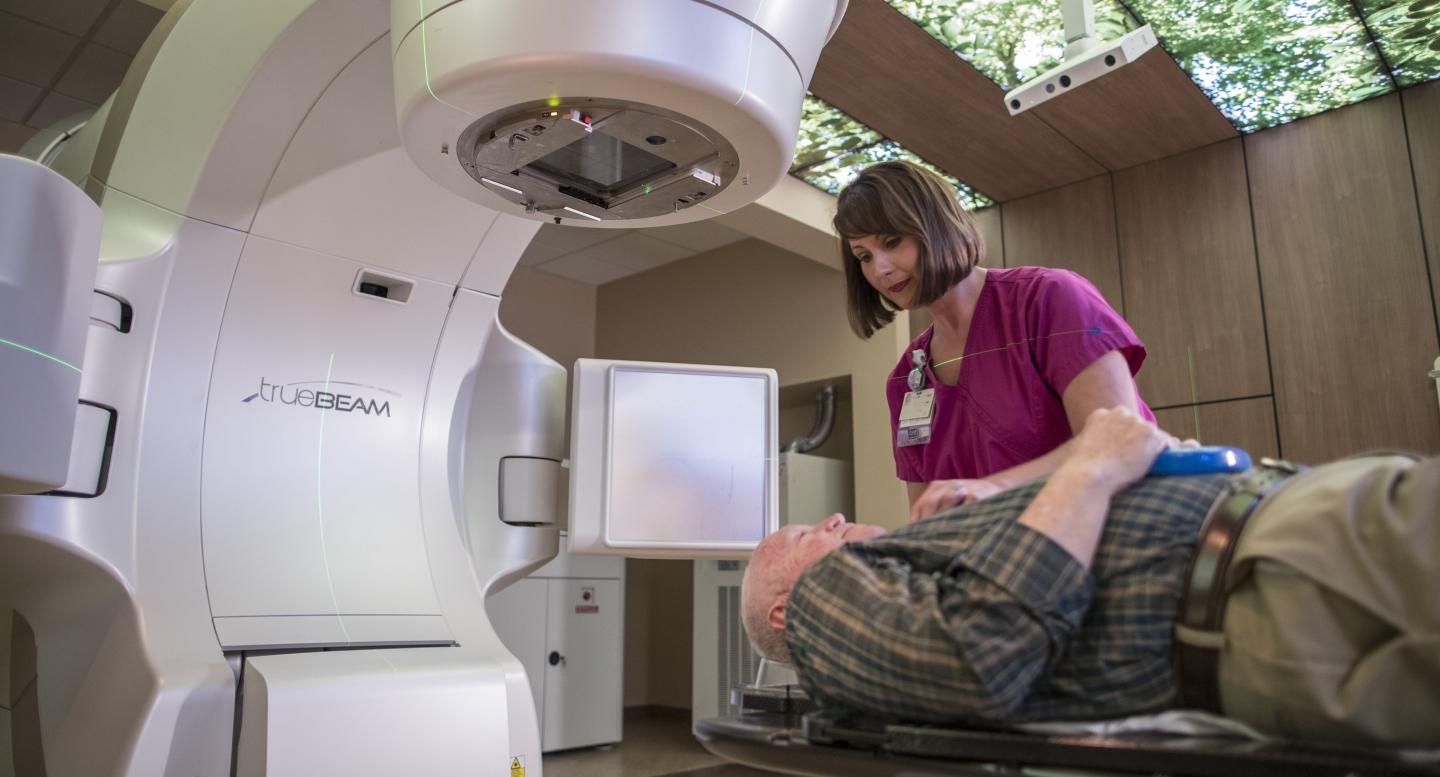
Treatment
You’ll get radiation on a machine called a linear accelerator, or linac for short. This machine makes the X-rays used to treat cancer. Before each session, your radiation therapist, or RT for short, will position you on the linac’s treatment table, or “couch.”
Once you’re in the right position, the therapist may use the machine to take a new image of the tumor. That will help them make sure it’s in the right position for that day’s treatment. During the imaging, the robotic imager arms on each side of the linac will stick out and begin to move in a circle around you. The RT may change your position so that it matches the position your team planned for you. The RT will leave the room before your treatment begins. You will be in constant contact with your RT through the cameras and microphones set up in the treatment room.
During the treatment, you will not see the radiation beam. You may hear the quiet buzz or shuffling of the beam-shaping device. It’s located inside the head, or gantry, of the machine. This beam-shaping device is called a multileaf collimator (MLC). It makes a uniquely shaped opening for the radiation beam to pass through. As the head, or gantry, rotates around you, it gives you radiation from different angles. The MLC continuously adjusts the beam. This lets it conform to, or match the shape of the tumor, and helps to deliver precise treatment. The linac will rotate around you as it delivers radiation right to the tumor.
Follow-Up Care
After you finish your treatment, your radiation oncologist and health care team will monitor your progress with a series of follow-up visits. These visits can include:
- A physical examination
- Blood screening
- More imaging
- Other tests that may be needed
Your follow-up appointments are also a good time for you and your caregivers to ask any questions about your progress. Your team can also answer questions about your overall health.
Use this information as a general guide to radiation therapy for cancer. It doesn’t replace a full discussion with your doctor and health care team. You should know that radiotherapy and radiosurgery aren’t appropriate for cancer types. Actual treatment times may vary. Patients usually get radiotherapy treatments once a day for a series of weeks. If you have radiosurgery, you’ll usually have it during one day or for a series of days. That depends on your particular case. You may have serious side effects like: diarrhea, nausea, swelling at the treatment site, lymphedema (swelling in the arms and legs) and secondary cancer. Talk to your doctor about what you can expect from your treatment. They will help you decide whether radiotherapy or radiosurgery are right for you.